INTRODUCTION
Cutaneous squamous cell carcinoma (cSCC) comprises 5% - 10% of eyelid and periorbital skin malignancies. Surgical excision is considered the first-line treatment of primary cSCC, and micrographically controlled surgery (MCS) has been pointed as the preferred choice in this sensitive anatomic location.1,2Nevertheless, these are time-consuming procedures that are not readily available, require reconstructive procedure, and are associated with recurrence.1 Topical photodynamic therapy (PDT), using a photosensitizing agent - methyl aminolevulinate (Metvix®) - is currently approved for the treatment of squamous cell carcinoma in situ.3 Therefore, it is reasonable to consider topical PDT as an alternative or additional option when dealing with preinvasive disease at this sensitive anatomic location.
Herein, we report a case in which topical PDT was used in the pe-riocular region to reduce the size of Bowen disease, before surgery, but revealed to be the best option for curative intent. Our report high-points the benefits of an integrative therapeutic approach to fulfill each patient’s individual needs.
CASE REPORT
A 61-year-old man had a punch biopsy-proven Bowen disease. The present lesion was extensive, measuring 40*25 mm in diameter, involving the left medial canthus, part of the lower and upper lid, and nasal dorsum (Fig.1). The remaining physical exam was normal. Initially, PDT was performed to reduce the size of the lesion before surgery. The procedure included scrapping all the affected areas to remove surface scaling. Subsequently, methyl aminole-vulinate 160 mg/g (Metvix®) cream was applied for a period of 3 hours before the light activation. A 10 mm rim of clinically normal skin was included. A dressing held the cream in situ and an eye protector was placed to cover the eye. After 3 hours, the cream was removed. The Aktilite CL128 was used for 7 minutes and 24 seconds (37 J/cm2). Each course of PDT consisted of two treatments, 1 week apart.
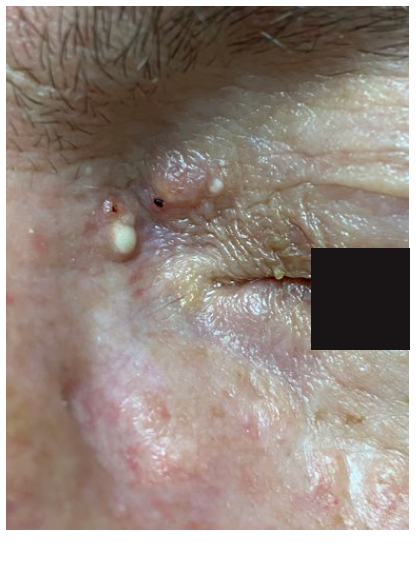
He underwent the first course of PDT in September of 2019. The reduction in the size of the lesion after the first treatment was significant. Despite the excellent results after the first course of PDT, the response was not complete, remaining a small papule in the upper eyelid (Fig. 2). He underwent another course of PDT in March of 2020. The only significant adverse effect reported was tolerable pain. The response was complete with an excellent aesthetic result. After 12 months of follow-up, no recurrence was observed (Fig. 3). A new skin biopsy ruled out residual disease (Fig. 4). He remains under follow-up.
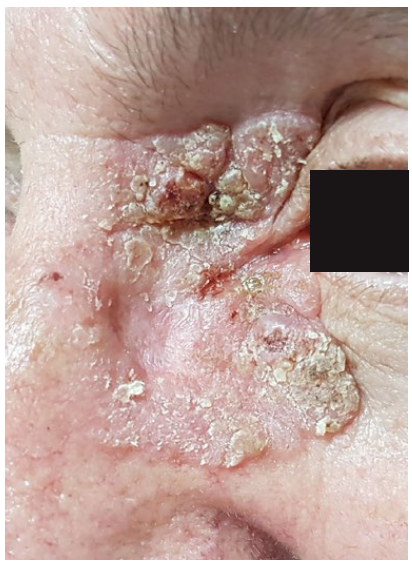
Figure 1 Skin-colored plaque, slightly desquamative, measuring 40*25 mm, involving the left medial canthus, lower and upper lid, and nasal dorsum.
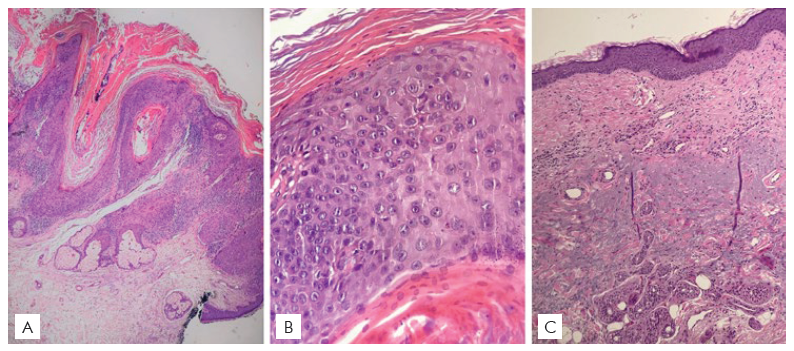
Figure 4 (A) Punch biopsy of a malignant proliferation of squamous cells in the epidermis and extending into follicular infundibula, with a verrucous pattern and associated with hyperkeratosis. (Hematoxylin-eosin stain; original magnification: x20). (B) The atypical squamous cells occupy the full thickness of the squamous layer, showing depolarization, irregular nuclear contour, increased nuclear/cytoplasmic ratio, and occasional binucleation. (Hematoxylin-eosin stain; original magnification: x40). (C) After treatment, the epidermis is flattened, with a regular squamous layer and normal cornification and without signs of malignancy. The papillary dermis is fibrotic, replacing and pushing down the elastotic fibers to the reticular dermis, consistent with post-treatment status. (Hematoxylin-eosin stain; original magnification: x40).
DISCUSSION
Published studies concerning PDT for periocular tumors are scarce. Almost all obtain some response and up to 42% of patients maintain response in long-term follow-up.4 Yet, we should be aware that these results usually refer to recurrent/persistent tumors treated with PDT.4,5The recurrence usually occurs within the first two years of follow-up. These recurrences might respond to another course of PDT. Moreover, PDT as neoadjuvant treatment allows more conservative surgery.4,5Treatment seems to be as well tolerated as at other sites with no long-term sequelae.4,5Even with MCS for primary periocular Bowen disease, the reported 5-year local recurrence rate is 2.5%.2
Our case reinforces PDT role in Bowen disease at the periocular area used as treatment or as a way for pre-surgical tumor debulking, thus reducing surgical morbidity. The final aesthetic and functional result may be excellent. Further studies are needed to establish the role and long-term results of PDT in similar clinical scenarios.
Presentations/Apresentações
Part of this work has been presented at the “1º Congresso Vir-tual de Dermatologia e Venereologia” in November of 2020.