Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Revista Portuguesa de Enfermagem de Saúde Mental
Print version ISSN 1647-2160
Revista Portuguesa de Enfermagem de Saúde Mental no.10 Porto Dec. 2013
Cognitive stimulation in elderly people
Estimulação cognitiva em idosos
Estimulación cognitiva en personas mayores
João Luís Alves Apóstolo*; Ana Isabel da Silva Rosa**; Inês Barata Sá Castro***; Daniela Filipa Batista Cardoso****
*RN; PhD; Adjunct Professor, Nursing School of Coimbra – Health Sciences Research Unit: Nursing, Avenida Bissaya Barreto - Apartado 7001, 3046-851 Coimbra, Portugal. E-mail: apostolo@esenfc.pt
**RN; Nursing School of Coimbra – Health Sciences Research Unit: Nursing, 3046-851 Coimbra, Portugal. E-mail: be.isrosa@gmail.com
***Grant holder, Nursing School of Coimbra – Health Sciences Research Unit: Nursing, 3046-851 Coimbra, Portugal. E-mail: castrines@gmail.com
****RN; Research Fellow, Nursing School of Coimbra – Health Sciences Research Unit: Nursing, Portugal Centre for Evidence-Based Practice: an Affiliate of the Joanna Briggs Institute, 3046-851 Coimbra, Portugal.E-mail: dcardoso@esenfc.pt
ABSTRACT
OBJECTIVES: To assess the effect of a cognitive stimulation programme (CSP) on the cognition of elders.
METHODS:One-group pretest-posttest study with two different samples, in different settings (studies 1 and 2) using a CSP. Study 1 took place in a Continuing Care Unit, with a sample of 13 inpatients (4 men and 9 women; mean age 66.90; SD 6.20 years). Study 2 took place in a Day Centre with a sample of 27 elders (8 men and 19 women; mean age 82.48; SD 7.06). One patient was excluded from sample 1 for not having completed the programme. Interventions were adjusted according to the participants’ impairments. The Portuguese version of Folstein’s Mini-Mental State Examination and Barthel ADL Index were used as pretest and posttest, and evolution was assessed through Wilcoxon Signed-Rank Test.
RESULTS: In study 1, 5 patients showed a negative evolution in cognitive function, 6 had a positive one, and 1 had no evolution. In study 2, there were 3 patients with a negative evolution, 14 with a positive one and 10 who maintained their cognitive functional level. In terms of autonomy in activities of daily living, study 1 had 9 negative evolutions, 1 positive one and 2 elders who maintained their status, whereas study 2 presented no differences in basicfunctional abilities between pretest and posttest.
CONCLUSIONS: Results point toward a positive effect of cognitive stimulation on the cognitive function of older adults. Therefore, CSPs should be included in older people’s health care regimens.
Keywords: Aged; Cognition; Dementia.
RESUMO
OBJETIVOS: Avaliar o efeito de um Programa de Estimulação Cognitiva (PEC) na cognição em idosos.
METODOLOGIA:Estudo pré-teste pós-teste em duas amostras diferentes, em diferentes contextos (estudos 1 e 2) usando um PEC. O estudo 1 decorreu numa Unidade de Cuidados Continuados, com uma amostra de 13 doentes (quatro homens e 9 mulheres; média de idades 66.90; SD 6.20 anos). O estudo 2 teve lugar num Centro de Dia com uma amostra de 27 idosos (8 homens e 19 mulheres; média de idades 82.48; DP 7.06). Um doente foi excluído da amostra 1 por não ter completado o programa. As intervenções foram ajustadas às incapacidades dos participantes. A versão Portuguesa do Mini-Mental State Examination de Folstein e Índice de Barthel foram usados como pré-teste e pós-teste, e a evolução foi avaliada pelo teste de Wilcoxon Signed-Rank.
RESULTADOS: No estudo 1, 5 doentes apresentaram uma evolução negativa na função cognitiva, 6 uma evolução positiva e 1 não teve evolução. No estudo 2, 3 idosos tiveram uma evolução negativa, 14 uma evolução positiva e 10 mantiveram o seu nível cognitivo funcional. Nas atividades de vida diária, o estudo 1 teve 9 evoluções negativas, 1 positiva e 2 idosos mantiveram o seu nível, enquanto no estudo 2 não apresentaram diferenças nas competências funcionais básicas entre o pré-teste e o pós-teste.
CONCLUSÕES: Os resultados apontam para um efeito positivo da estimulação cognitiva na função cognitiva de idosos. Portanto, os PECs devem ser incluídos nos cuidados de saúde.
Palavras-chave: Idoso, Cognição, Demência.
RESUMEN
OBJETIVOS: Evaluar el efecto de un Programa de Estimulación Cognitiva (PEC) en la cognición de personas mayores.
METODOLOGÍA: Pre-test y post-test con dos muestras distintas en diferentes contextos (Estudios 1 y 2) con un PEC. Se realizó el estudio 1 en una Unidad de Cuidados Continuos, con una muestra de 13 pacientes (4 hombres y 9 mujeres; media de 66,90 años, DP 6,20 años). Se llevó a cabo el estudio 2 en un centro de día con una muestra de 27 adultos mayores (8 hombres y 19 mujeres; media de 82,48 años, DP 7.06). Un paciente fue excluido de la muestra 1 por no haber completado el programa. Se ajustaron las intervenciones a las discapacidades de los participantes. Se utilizó la versión en portugués del Mini Examen del Estado Mental de Folstein y el índice de Barthel como pre-test y post-test. El resultado se evaluó mediante el Wilcoxon Signed-Rank.
RESULTADOS: En el estudio 1, 5 pacientes experimentaron una evolución negativa en la función cognitiva; 6 positiva y 1 sin evolución. En el estudio 2, 3 ancianos tuvieron una evolución negativa; 14 positiva y 10 mantuvieron su función cognitiva. Con respecto a actividades de la vida diaria, en el estudio 1 se registraron 9 evoluciones negativas, 1 positiva y 2 ancianos mantuvieron su nivel, mientras que el estudio 2 no reveló diferencias en las actividades de la vida diaria entre el pre -test y post -test.
CONCLUSIONES: Los resultados indican un efecto positivo de la estimulación cognitiva en la función cognitiva de los ancianos. Por lo tanto, los PEC deben ser incluidos en el cuidado de la salud.
Descriptores: Anciano; Cognición; Demencia.
Introduction
Population aging has led to an increased prevalence of chronic degenerative diseases, particularly dementia. In 2010, an estimated 35.6 million people worldwide lived with dementia. This number is estimated to nearly double every 20 years and much of the increase is attributable to increases of people with dementia in low and middle income countries (Prince & Jackson, 2009). The total estimated worldwide costs of dementia were US$604 billion in 2010, and about 70% of these occurred in Western Europe and North America (Wimo & Prince, 2010).
Mild cognitive impairment (MCI) is increasingly recognized as an important public health issue since it can be associated to an increased risk of developing dementia. Annual conversion rates vary across different studies with clinical samples showing higher rates of conversion than community-based samples. One study (Mitchell & Shiri-Feshki, 2009) using Mayo-defined MCI identified forty-one robust cohort studies and the cumulative proportions of MCI that progressed into dementia, Alzheimer’s disease (AD) and vascular dementia (VaD) were, respectively, 39.2%, 33.6% and 6.2% in specialist settings, and 21.9%, 28.9% and 5.2% in population studies. The adjusted annual conversion rate (ACR) from Mayo-defined MCI conversion into dementia, AD, and VaD, was 9.6%, 8.1% and 1.9%, respectively, in specialist clinical settings and 4.9%, 6.8% and 1.6% in community studies (Mitchell & Shiri-Feshki, 2009).
In the United Kingdom, the National Institute for Health and Clinical Excellence and the Social Care Institute for Excellence (NICE-SCIE) clinical guidelines on dementia recommend that people with mild/moderate dementia should be given the opportunity to participate in a structured group cognitive stimulation programme (National Institute for Health, Clinical Excellence and the Social Care Institute for Excellence, 2006).
The maintenance of cognitive health is of vital importance for the quality of life of older adults and their relatives. Several studies have provided statistical evidence that cognitive stimulation helps to improve the cognitive function of elders with or without cognitive impairment. Social engagement, physical activity, leisure activities, and cognitive stimulation contribute to an increase in the brain’s synaptic density - responsible for brain dynamics and plasticity - and cognitive reserve, thus offering protection against the clinical symptoms of dementia (Butters et al., 2008; Hertzog, Kramer, Wilson & Lindenberger, 2008; La Rue, 2010; Souza & Chaves, 2005; Yassuda, Batistone, Fortes & Neri, 2006). Not only do these activities keep elders mentally active while having an enjoyable time, but they also help to preserve or enrich their cognition.
Evidence also suggests positive effects of cognitive stimulation when combined with cholinesterase inhibitor medication (Jean, Bergeron, Thivierge & Simard, 2010; Spector, Woods & Orrell, 2008; Yassuda et al., 2006). Dementia and other aging-related cognitive disorders are extremely expensive in terms of financial resources invested in health care, morbidity, mortality, and carers’ disorders. Therefore, cognitive stimulation can have a good cost-benefit ratio. In dementia, the benefits in cognition are comparable to those obtained through medication (Knapp et al., 2006; Spector et al., 2008)
A literature review suggested that participating in cognitive leisure activities, either during mid life or late life may have a protective effect on the prevention of dementia (Stern & Munn, 2010). However, they advise caution when interpreting results due to the quality of the included studies, particularly their design and the heterogeneity of population and interventions.
In Portugal, there is a need for research concerning the cognitive health of institutionalized elders, and for the development of cognitive stimulation programmes. Taking this into account, the aim of this study is to assess the effect of a stimulation programme on the cognitive functions of elders.
Methodology
Design
In order to measure cognition differences between two different samples, in different settings (referred to as study 1 and study 2), a one-group pretest-posttest study was conducted.
Inclusion criteria
Both studies included the older adults (over 65 years) using these services who agreed to participate in the programme and whose physical condition (such as sensory impairment or high level of agitation) or cognitive impairment did not impede participation. This was determined using Barthel Index and Mini-Mental State Examination (MMSE): people who scored 20 or less in Barthel Index (totally dependent) or who scored 10 or less in MMSE (severe cognitive impairment) were excluded.
Setting and Sample
Study 1: 13 elderly inpatients in a long-stay continuing care unit in the Centre region of Portugal. The sample was composed of 4 men and 9 women, aged between 65 and 87 years (mean age: 66.90 years; SD: 6.20 years). In the posttest, one patient was excluded from the sample for not having completed the intervention programme due to worsening of his clinical symptoms.
Study 2: 27 elders attending a day center in the Center region of Portugal. The sample was composed of 8 men and 19 women, aged between 65 and 99 years (mean age: 82.48 years; SD: 7.06 years).
Instruments
The Portuguese versions of Folstein’s MMSE (Guerreiro, Silva, Botelho, Leitão, Castro-Caldas & Garcia, 1994) and of the Barthel ADL Index (Araújo, Ribeiro, Oliveira & Pinto 2007) were used as pretest and posttest in both studies.
Intervention
A cognitive stimulation programme was developed and implemented by the researchers, supported by the local teams of nurses and final-year students (4th year) of the nursing undergraduate course who had received proper training to apply it.
Study 1 took place from October 2009 to January 2010, with 4 sessions per week. Study 2 took place from April to June 2010, and included 3 sessions per week. In both studies each session lasted between 1 and 1.5 hours.
The intervention programme was composed of several exercises adjusted to the participants’ impairments, stimulating different areas: attention, language, gnosia, memory, praxia, and executive functions.
Exercises included reading, interpretation and reference to texts; sentence ordering; construction of action sequences; similarities and differences between figures; arithmetic calculus; identification of objects, their gender and antonyms; identification of textures, sounds, images and smells; sentence completion; selection of figures, numbers and words; memorization of shopping lists; use of personal stories; mimics; copy of drawings; painting; ball game; proverbs and metaphors.
Statistical methods
The statistical methods used included the determination of descriptive statistics and application of Wilcoxon Signed-Rank Test (Siegel, 1975) using the SPSS 19 software. P-values of less than 0.05 were considered significant.
Ethical Considerations
The study was approved by the Ethical Committee of the Health Sciences Research Unit: Nursing of the Nursing School of Coimbra (Nº P12-11/2010). Institutional review board approval was granted and participants (or the participant's legally authorized representative) signed an informed consent prior to completing the baseline assessment.
Results
Study 1
Basic functional abilities: Barthel Index assessed in the pretest revealed 8 participants with severe dependence, 3 with moderate dependence, 1 with mild dependence and 1 independent. Wilcoxon Signed-Rank Test (pretest-posttest) showed 9 negative ranks (Mean Rank 5.11), 1 positive rank (Mean Rank 9.00) and 2 ties (z=-1.896; p=0.058).
Cognition: MMSE used in the pretest assessed 6 participants with "normal" cognition and 7 with cognitive impairment. Results of Wilcoxon Signed-Rank Test are presented in the Table 1.
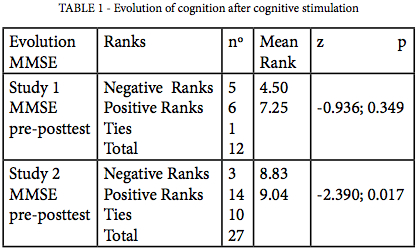
Study 2
Basic functional abilities: Pretest using Barthel Index assessed 3 participants with severe dependence, 8 with moderate dependence, 7 with mild dependence and 9 independent. No differences were found in basicfunctional abilities between pretest and posttest.
Cognition: pretest MMSE assessed 20 participants as having "normal" cognition and 7 with cognitive impairment. See Table 1 for the results of Wilcoxon Signed-Rank Test.
Discussion
Both studies had limitations, namely the lack of control groups, and the differences between studies 1 and 2 that hamper the comparison of results from both groups.
Furthermore, study 1 used a very small sample making statistical inference unreasonable - although a statistically irrelevant outcome is not necessarily a clinically irrelevant one (Loureiro & Gameiro, 2011). It should be stressed that, in this study, patients were hospitalized in a long-stay Continuing Care Unit because their clinical or social condition did not allow them to stay in their homes and the sample was mainly composed of severely dependent people. Three of these patients presented a worsening of their clinical status, particularly due to respiratory infections, which may have limited the effectiveness of the stimulation programme.
In study 2 better results were obtained in spite of the fact that the programme was implemented for a shorter period of time, fewer times per week, and the sample was generally composed of older people (mean age of 82.48 years, in comparison to the mean age of 66.90 in study 1).
Because long-term outcomes are still controversial, further studies ought to include maintenance interventions and follow-up assessments as well as the use of larger samples and control groups, as previously mentioned.
Overall, we consider the intervention had positive outcomes because even small improvements or the stabilization of cognitive functions can be considered significant health gains.
These results are in agreement with the conclusions drawn from a recent systematic review (Jean et al., 2010), which addressed the efficacy of 15 cognitive intervention programmes tested in individuals with mild cognitive impairment of the amnestic type (MCI-A) at risk of possibly progressing toward dementia. Statistically significant improvements after treatment were obtained on 49% of subjective measures of memory, quality of life, or mood. Sample sizes ranged from 1 to 193 patients with MCI-A, but were usually inferior or equal to 30. Five studies were randomized controlled trials, eight were quasi-experimental designs, and two were single-case investigations. Despite the heterogeneity of studies and the fact that just below 50% of cases proved to be effective, these results are encouraging, not only because of the good cost-benefit relation that this type of interventions present (Knapp et al., 2006), but also because of the importance for elders (and their families) to avoid dementia as much as possible.
Conclusion
Although statistical inference from the data obtained might be risky, our results point toward a positive effect of cognitive stimulation on the cognitive function of older adults. Small improvements and the stabilization of cognitive functions can be considered significant health gains.
Cognitive stimulation should be included in older people’s health care regimens because it may preserve their cognitive and functional abilities and one might expect that, as a result, it could contribute to a higher level of autonomy. In particular, people with mild-to-moderate cognitive impairment should be given the opportunity to participate in a structured group cognitive stimulation programme.
References
Araújo, F., Ribeiro J. L. P., Oliveira A., & Pinto C. (2007). Validação do Índice de Barthel numa amostra de idosos não institucionalizados. Revista Portuguesa de Saúde Pública, 25(2), 59-66. [ Links ]
Butters, M. A., Young, J. B., Lopez, O., Aizenstein, H. J., Mulsant, B. H., Reynolds III, C. F., DeKosky, S. T., & Becker, J. T. (2008). Pathways linking late-life depression to persistent cognitive impairment and dementia. Dialogues in clinical neuroscience, 10(3), 345-357. [Consult. 16-2-2011]. Retrieved from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2872078/ [ Links ]
Guerreiro, M., Silva A. P., Botelho M. A., Leitão O., Castro-Caldas A., & Garcia C. (1994). Adaptação à população portuguesa da tradução do "Mini Mental State Examination" (MMSE). Revista Portuguesa de Neurologia, 1, 9-10. [ Links ]
Hertzog, C., Kramer, A. F., Wilson, R. S., & Lindenberger, U. (2008). Enrichment Effects on Adult Cognitive Development Can the Functional Capacity of Older Adults Be Preserved and Enhanced?. Psychological Science in the Public Interest, 9(1), 1-65. [ Links ]
Jean, L., Bergeron, M. È., Thivierge, S., & Simard, M. (2010). Cognitive intervention programs for individuals with mild cognitive impairment: systematic review of the literature. American Journal of Geriatric Psychiatry, 18(4), 281-296. [ Links ]
Knapp, M., Thorgrimsen, L., Patel, A., Spector, A., Hallam, A., Woods, B., & Orrell, M. (2006). Cognitive stimulation therapy for people with dementia: cost-effectiveness analysis. The British Journal of Psychiatry, 188(6), 574-580. [ Links ]
La Rue, A. (2010). Healthy brain aging: role of cognitive reserve, cognitive stimulation, and cognitive exercises. Clinics in geriatric medicine, 26(1), 99-111. [ Links ]
Loureiro, L. M., & Gameiro, M. G. H. (2011) Interpretação crítica dos resultados estatísticos: para lá da significância estatística. Journal of Nursing Referência, III(3), 151-162. [ Links ]
Mitchell, A. J., & Shiri‐Feshki, M. (2009). Rate of progression of mild cognitive impairment to dementia–meta‐analysis of 41 robust inception cohort studies. Acta Psychiatrica Scandinavica, 119(4), 252-265. [ Links ]
National Institute for Health, Clinical Excellence and the Social Care Institute for Excellence (2006). Dementia: supporting people with dementia and their carers in health and social care. London: NICE, SCIE. [ Links ]
Prince, M., & Jackson, J. (2009). World Alzheimer Report 2009. [online] London: Alzheimer's Disease International. Retrieved from: http://www.alz.co.uk/research/files/WorldAlzheimerReport.pdf [ Links ]
Siegel S. (1975). Estatística não-paramétrica para ciências do comportamento (Nonparametric Statistics for The Behavioral Sciences). Trad. Alfredo Alves de Farias. São Paulo: McGraw-Hill. [ Links ]
Souza, J. N., & Chaves, E. C. (2005). O efeito do exercício de estimulação da memória em idosos saudáveis. Revista da Escola de Enfermagem da USP, 39(1), 13-19. Retrieved from: http://www.ee.usp.br/reeusp/upload/pdf/40.pdf [ Links ]
Spector, A., Woods, B., & Orrell, M. (2008). Cognitive stimulation for the treatment of Alzheimer’s disease. Expert Review of Neurotherapeutics, 8(5), 751-757.
Stern, C., & Munn, Z. (2010). Cognitive leisure activities and their role in preventing dementia: a systematic review. International Journal of Evidence‐Based Healthcare, 8(1), 2-17. [ Links ]
Wimo, A., & Prince, M. J. (2010). World Alzheimer Report 2010: the global economic impact of dementia. [online]. London: Alzheimer's Disease International. Retrieved from: http://www.alz.co.uk/research/files/WorldAlzheimerReport2010.pdf [ Links ]
Yassuda, M. S., Batistoni, S. S. T., Fortes, A. G., & Neri, A. L. (2006). Treino de memória no idoso saudável: benefícios e mecanismos. Psicologia: reflexão e crítica, 19(3), 470-481. [ Links ]
Recebido em 30 de agosto de 2013.
Aceite para publicação em 25 de novembro de 2013.