Introduction
The primary malignant cancer of the Fallopian tube is one of the rarest gynecological cancers and represents less than 1% of all cancers of the female genital system1.
The main histological type is serous epithelial and appears most frequently in the fifth and sixth decades of life. Its etiopathogenesis remains little known. Hormonal, reproductive and genetic factors seem to have an important contribution4. Women with mutations in the BRCA1 and BRCA2 genes have been shown to have a considerable risk of developing tube cancer1.
Although the incidence of this cancer is very low, it is considered that this value is underestimated. Many high-grade serous carcinomas (HGSC) of the tube have been classified as cancers of the ovary, when in the light of current scientific evidence, they are likely to be primary cancers of the tube. We are witnessing a paradigm shift, in which the Fallopian tube is considered the primary site of most HGSC. During more than 30 years, the prevailing view on the origin of HGSG was that it derived from the ovary, since the ovarian surface epithelium is exposed to inflammation and oxidative stress induced by ovulation. At the beginning of this century, many studies were published demonstrating the presence of invasive and non-invasive cancer in the Fallopian tubes of prophylactic salpingo-oophorectomies performed in carriers of BRCA mutation, which led some authors to suggest the tube as the origin of these cancers. The precursor lesion - serous tubal intraepithelial cancer - was described. The advances in cellular and molecular biology and in genetics added support for this new concept, indicating that the HGSC develops from an occult intraepithelial cancer in the fimbria of the tube and involves the ovary secondarily5.
Normally, the clinical manifestations of the tube cancer appear earlier than in malignant ovarian cancers, due to abdominal pain secondary to tubal distention. The classic Latzko triad of signs and symptoms associated with the tube cancer includes: intermittent sero-hematic vaginal discharge (hydrops tubae profluens), colic-type abdominal pain and a palpable adnexal mass. However, this triad is only found in less than 15% of patients and the evolution is usually asymptomatic1;5;11.
Preoperative diagnosis is difficult, since the cancer course is usually silent, and the signs and symptoms are not specific. Even so, they are diagnosed at an earlier stage than ovarian cancer.
The differential diagnosis criteria for tube cancer, currently, include: 1. The dominant mass is located in the tube and grows from its lumen; 2. There is histological evidence of transition between carcinoma in situ and invasive cancer, in the tubar epithelium; 3. The ovaries and endometrium must be normal or contain fewer cancer cells than those found in the tube; 4. The histological pattern reproduces the epithelium of the tubal mucosa2;4;5.
Breast metastasis of gynecological cancer is mainly described as associated with ovarian cancer. Very few cases of breast metastases originating from a primary malignant cancer of the tube have been reported, and this association is therefore considered to be very rare.
We describe what, to our knowledge, is the fifth reported clinical case of breast metastasis from a primitive serous adenocarcinoma of the Fallopian tube.
Clinical case
Female patient, 61 years old, caucasian, was referred to the emergency department for chest pain with pleuritic characteristics, fatigue and dyspnoea.
A chest CT scan was performed, which revealed massive pericardial effusion and bilateral pleural effusion. An evacuation puncture of the pericardial effusion was performed, which demonstrated the presence of cancerous cells. The abdominal-pelvic CT scan revealed a cystic formation in the left ovary, with regular contours and homogeneous characteristics. Adenopathies were also observed in the right iliac chain, as well as peritoneal effusion. Ca-125 was 4249 U/ml.
An exploratory staging laparotomy was performed, due to suspected ovarian cancer. She underwent primary surgery with maximum tumor cytoreduction, with total hysterectomy, bilateral annexectomy, excision of peritoneal metastases, pelvic lymphadenectomy and infra-colic omentectomy.
The left annexectomy piece had a tubal cancer developed from the tube's mucosa, completely occupying its lumen, destroying the mucosa and massively infiltrating the pear-tubar tissue, reaching the margin of surgical resection. The cancer mostly had a glandular, fenestrated and papillary pattern. There was also the presence of cancer lymphatic embolization in the pear-tubar tissue. The left ovary and the right annexectomy piece did not present cancerous infiltration.
Thus, in 2007, serous adenocarcinoma of the Fallopian tube, already in stage IV of FIGO, was diagnosed by pericardial metastasis with cardiac tamponade.
The patient underwent 6 cycles of 1st line palliative chemotherapy with Paclitaxel and Carboplatin but remained with residual disease. She was asymptomatic and with imaging without signs of illness. In 2008, she had a recurrence of the disease having undergone 3 cycles of 2nd line palliative chemotherapy with Carboplatin and Cyclophosphamide, which was suspended due to toxicity (severe nausea and vomiting), keeping under clinical surveillance.
Six months after the interruption of 2nd line chemotherapy, and 2 years after the diagnosis of primitive fallopian tube cancer, the patient detected a nodule in the right breast. She underwent a mammogram, which revealed a dense nodular formation, with poorly defined contours and edema of the subcutaneous tissue. She underwent breast ultrasound that confirmed a solid and hypoechogenic, irregular nodular formation in the infero-internal quadrant.
Echo-guided microbiopsy of the breast cancer was performed. The histological study showed cancerous lesions with papillary pattern, branched fibrovascular axes, with marked retraction of the surrounding stroma, desmoplastic reaction and images of cancer lymphatic embolization. Thus, the morphological and immunohistochemical aspects were compatible with metastasis to the right breast of the primitive serous cancer of the tube.
Since then, there has been a progressive worsening of her general condition, having undergone a chest CT scan that revealed irregular pleural thickening with small subpleural nodular formations compatible with secondary locations, thickening of interlobular septa and bilateral hilar peri-bronchovascular thickening.
About a month after having undergone the biopsy of the breast nodule, in a Therapeutic Decision Meeting, due to the poor general condition, the patient was considered without the possibility of specific treatment and was referred to the Palliative Care Unit, dying on the seventh day of hospitalization.
Discussion
The primary malignant cancer of the Fallopian tube is a rare entity2. Its histology and biological behavior are similar to those of ovarian cancer, so the staging and treatment of these cancers are essentially the same1.
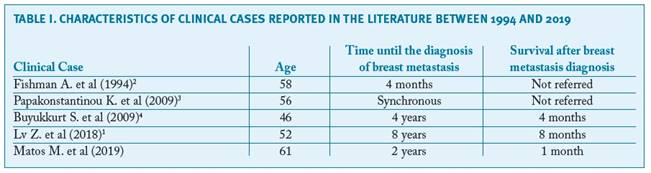
The breast is an uncommon location for metastatic malignancy. Its frequency varies between 0.5% and 1.3%3. The malignant cancers that most often metastasize to the breast are lymphoma and melanoma14. Since the first case of breast metastasis of a primary tube cancer was reported in 1994, only four similar cases have been described in the world literature (Table I). In all cases in which this metastasis occurred, the disease was already widespread.
Breast metastases can be caused by hematogenous or lymphatic routes, both with different clinical characteristics. In general, secondary cancers that originate by hematogenous dissemination, appear as a well circumscribed, oval mass, without a desmoplastic reaction. In the case of primary serous cancers of the tube and ovary, metastasis appears to be more common via the lymphatic route, characterized by a unique nodular formation of ill-defined contours and edema of the underlying subcutaneous cell tissue, retraction of the skin or nipple, breast discharge and sign of peau d'orange and microcalcifications on mammography (due to the presence of psamomatous bodies)4;7.
In the clinical case presented, the initial diagnosis pointed to ovarian cancer, as in the cases published by Papakonstantinou K. et al and Buyukkurt S. et al, who reported two cases whose initial suspected diagnosis was also malignant cancer of the ovary.
In the case reported by Papakonstantinou K. et al, there was a synchronous presentation of the primary tube cancer with breast metastasis. This situation is unusual, as it tends to occur later in the natural history of the disease4;5. Fishman A. et al described a case of breast metastasis and homolateral axillary ganglion involvement, detected four months after the diagnosis of a primary tube cancer3. It was reported by Lv Z. et al a case of breast metastasis and ganglion involvement, detected eight years after the diagnosis of a primary cancer8. A case of synchronous breast and cardiac metastasis, detected four years after the diagnosis of a primary cancer, was reported by Buyukkurt S. et al7.
In the present clinical case, breast metastasis arose about two years after the diagnosis of a primary Fallopian tube cancer, in a setting of multiple metastasis and in the absence of response to chemotherapy.
Despite its rarity, breast metastasis is a sign of poor prognosis for oncological disease and is associated with multiple cancer metastasis.
The presence of residual disease after surgery is an important prognostic factor that reduces life expectancy. The stage of the cancer at the time of diagnosis is the most important prognostic factor13. The survival rate after the diagnosis of a breast metastasis appears to be very variable, ranging from just 13 days to 3.5 years6;7. In the case presented by us, the survival after histological diagnosis of breast metastasis was one month (Table 1).