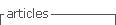Services on Demand
Journal
Article
Indicators
-
 Cited by SciELO
Cited by SciELO -
 Access statistics
Access statistics
Related links
-
 Similars in
SciELO
Similars in
SciELO
Share
Acta Obstétrica e Ginecológica Portuguesa
Print version ISSN 1646-5830
Acta Obstet Ginecol Port vol.12 no.2 Coimbra June 2018
ISSUE IMAGE/IMAGEM DO TRIMESTRE
Spina bifida detection in first trimester ultrasound
Diagnóstico de espinha bífida na ecografia do primeiro trimestre
Eliana Teixeira*, Rui Marques Carvalho**, Nuno Clode***
Centro Hospitalar Lisboa Norte - Hospital de Santa Maria
*Interna de Ginecologia e Obstetrícia, Centro Hospitalar Barreiro Montijo
**Assistente Hospitalar de Ginecologia e Obstetrícia, Clínica Universitária de Obstetrícia e Ginecologia do Centro Hospitalar Lisboa Norte (Hospital de Santa Maria)
***Diretor de Serviço de Obstetrícia, Clínica Universitária de Obstetrícia e Ginecologia do Centro Hospitalar Lisboa Norte (Hospital de Santa Maria)
Endereço para correspondência | Dirección para correspondencia | Correspondence
ABSTRACT
Spina bifida is one of the most common severe congenital defects of the central nervous system. Prenatal diagnosis is currently performed in second trimester. First trimester diagnosis is rare and can be challenging, but it can be suspected in the absence of intracranial translucency.
We report images of a case of spina bifida detected at 13 weeks scan. The fetus presented images suggestive of open spina bifida and intracranial translucency was absent, also the crown-rump length evolution in serial ultrasound examinations was deficient. At 16 weeks a spontaneous abortion occurred and the histopathology analysis confirmed the diagnosis of spina bifida.
Keywords: Spina bifida; First trimester; Intracranial translucency.
Neural tube defects (NTDs) are the second most common congenital anomaly worldwide1 and are associated with severe central nervous system disability. The incidence varies according to race, geographic region and socioeconomic status and usually ranges from <1 to 7 per 1000 live births2,3. Anencephaly and spina bifida are the most common NTDs2.
Currently, prenatal diagnosis of spina bifida is mainly performed in the second trimester screening and relies on the observation of the fetal spine and recognition of associated skull and brain abnormalities, secondary to Arnold-Chiari malformation. This malformation is thought to be a consequence of the leakage of cerebrospinal fluid into the amniotic cavity and hypotension in the subarachnoid spaces leading to caudal displacement of the brain and obstructive hydrocephalus, with obliteration of the cisterna magna. As a result of this mechanism, absence of the intracranial translucency (IT) in the first trimester screening may be seen in fetuses with open spina bifida4,5. Intracranial translucency, assessed in the mid-sagittal view of the posterior brain, is delineated by two echogenic borders: the dorsal part of the brain stem anteriorly and the choroid plexus of the fourth ventricle posteriorly4. IT represents the fourth ventricle and is easily visible in normal fetuses.
Some studies reported that evaluation of fetal IT is a valuable sonographic landmark that can improve early detection rates of open spina bifida. However, further data on sensitivity and specificity and larger prospective studies are still needed.
The images below show a case of a fetus with open spina bifida and absence of intracranial translucency detected at 13 weeks ultrasound scan.
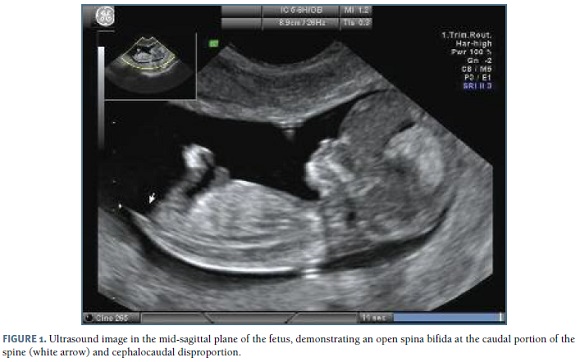
A healthy 37- year-old primipara, with no risk factors to NTD and with the recommended folic acid intake, presented at 10 weeks gestation for ultrasound examination at our institution. At this time the crown-rump length (CRL) was 33.6mm and at 12 weeks of gestation the evolution was only to 44.5mm. At 13 weeks a new ultrasound scan was performed, at this time the biparietal diameter was between the normal ranges (18.4mm) but the fetus continued smaller than expected, the CRL was 51.6mm. Nuchal translucency was within the normal limits (1.24mm). During this exam a lumbosacral open spina bifida was detected (Figure 1) and routine examination of the posterior brain showed the absence of intracranial translucency. Prenatal counselling was made, recommending genetic counselling and an invasive diagnostic test, but it was refused by the couple that decided to proceed the pregnancy, only with ultrasound examinations. At 16 weeks of gestation a spontaneous abortion occurred and the histopathology analysis reported a depression of the skin and vertebrae at the lumbosacral level, confirming the spina bifida diagnosis. All the anthropometric parameters were concordant but inferior to 11 weeks of gestation. Other morphological anomalies were excluded.
This case illustrates that the diagnosis of open spina bifida in the first trimester screening is possible and demonstrates the increasing importance of intracranial translucency in early diagnosis.
REFERENCES
1. Neural tube defects. ACOG Practice Bulletin No. 44. American College of Obstetricians and Gynecologists. Obstet Gynecol 2003; 102:203-13. [ Links ] (Reaffirmed in 2014).
2. Khoshnood B, Loane M, De Walle H, Arriola L, Addor MC, Barisic I, et al. Long term trends in prevalence of neural tube defects in Europe: population based study. BMJ 2015; 351:h5949. [ Links ]
3. McLone D, Bowman R. Pathophysiology and clinical manifestations of myelomeningocele (spina bifida). In: UpToDate, Post TW (Ed), UpToDate, Waltham, MA. Accessed on December 8, 2016. [ Links ]
4. Chaoui R, Benoit B, Mitkowska-Wozniak H, Heling KS, Nicolaides KH. Assessment of intracranial translucency (IT) in the detection of spina bifida at the 11-13-week scan. Ultrasound Obstet Gynecol 2009; 34: 249-252. [ Links ]
5. Chaoui R, Nicolaides KH. From nuchal translucency to intracranial translucency: towards the early detection of spina bifida. Ultrasound Obstet Gynecol 2010; 35: 133-138. [ Links ]
Endereço para correspondência | Dirección para correspondencia | Correspondence
Eliana Teixeira
Centro Hospitalar Barreiro Montijo EPE
Portugal
E-Mail: elianapteixeira@gmail.com
Recebido em: 04/02/2017
Aceite para publicação: 22/07/2017